Original Article: JRCRS. 2026:14(1):17-22
4-Effect of Lumber Sustained Natural Apophyseal Glides on Lower Cross Syndrome: A Randomized Controlled Trial
Amreen Shabbir1, Sidra Asghar2, Rabbiya Atta Qazi3, Aniqa Khalid4, Jassia Ramzan5, Ayesha Saddiqa6
1 2 4 5 6 Lecturer, Mohi-u-Din Institute of Rehabilitation Sciences, Mohi-u-Din-Islamic University, Mirpur AJK, Pakistan
3 Assistant Professor, Mohi-u-Din Institute of Rehabilitation Sciences, Mohi-u-Din-Islamic University, Mirpur AJK, Pakistan
Full-Text PDF DOI: https://dx.doi.org/10.53389/JRCRS.2026140104
ABSTRACT:
Background: Lower cross syndrome, also referred to as pelvic crossed syndrome, develops when insufficient muscle strength causes an imbalance in the lower extremities. It is marked by a pattern of weakness and tightness between opposing muscle groups on the front and back of the body. Lumbar sustained natural apophyseal glides (SNAGs) are a mobilization technique used to reduce pain, correct hypomobility and biomechanical faults such as anterior pelvic tilt and hyperlordosis, and improve posture and function.
Objective: To determine the effect of lumbar SNAGs on pain and hypomobility in individuals with Lower Cross Syndrome.
Methodology: A randomized controlled trial was conducted at Gulam Abbas Orthopedic Hospital, kotli, Azad Kashmir and the District Headquarter Hospital, kotli Azad Kashmir, with a sample size of 36 participants determined by G*Power (effect size 0.25, α = 0.05, power = 0.95). Participants were allocated into two group using non-probability purposive sampling technique Group A (lumbar SNAGs plus moist heat, stretching tight erector spinae, hip flexors and strengthening of weak abdominals and gluteal muscles) and Group B (moist heat with stretching tight erector spinae, hip flexors and strengthening of weak abdominals and gluteal muscles only, with 5-7 reps of 1 set of each exercise, delivered three times a week for three weeks. Pain was assessed using the Numeric Pain Rating Scale and lumbar range of motion using goniometer. (Clinical Trial Registry Number: (NCT06707805)
Results: Between-group analysis demonstrated statistically significant effects of lumbar SNAGs combined with conventional therapy, showing a reduction in pain intensity (p < 0.05) and an improvement in lumbar range of motion (p ≤ 0.05).
Conclusion: This study concludes that the addition of lumbar SNAGs to conventional therapy produces clinically meaningful improvements in pain reduction and lumbar mobility compared with conventional therapy alone, in the management of patients with lower-crossed syndrome.
Keywords: Conventional therapy, Lumbar SNAGs, Lower cross syndrome, NPRS, ROM.
Introduction:
Lower cross syndrome, also referred to as pelvic crossed syndrome, develops when insufficient muscle strength causes an imbalance in the lower extremities. It is marked by a pattern of weakness and tightness between opposing muscle groups on the front and back of the body. Commonly, the abdominal muscles along with the gluteus maximus and gluteus medius are weak, while the hip flexor muscles are excessively tight.1
Lower cross syndrome affects several key muscle groups, including the oblique and rectus abdominis, gluteus maximus, gluteus medius, and hamstrings. In addition, the iliopsoas, rectus femoris, tensor fascia lata, adductor muscles, gastrocnemius, and soleus are also involved.2
The development of lower cross syndrome results in an anterior pelvic tilt, exaggerated lumbar curve, hip flexion, and knee hyperextension.3 Lower cross syndrome may develop due to various factors, such as repetitive or prolonged running activities. Physical inactivity can adversely affect the body’s mechanics through factors such as immobilization, muscle disuse, or ongoing postural pain, while prolonged sitting and poor workplace posture can further contribute to these issues.2 Pain in one or both legs is frequently present, and some patients with pain in their low back also experience neurological symptoms in their lower limbs.4 Low back pain is especially common during adolescence, with its highest prevalence occurring in the third decade of life.3 Researchers investigated the prevalence of lower cross syndrome among school-aged children (11–15 years) and found that 21% participants showed clinical signs of the condition, while an additional 32% were considered at risk. Assessments using manual muscle testing and flexibility measures also revealed sex-based differences, with 22% of boys and 18% of girls being affected.5
The most frequent reason patients visit the hospital emergency room is for back pain.6 Exercises are commonly employed to address postural deviations by lengthening tight structures and reinforcing weak muscle groups. Corrective exercise programs work by stimulating skeletal muscles to guide body segments toward proper alignment.7
This study aims to evaluate the effectiveness of lumbar SNAGs in managing LCS by assessing their impact on pain, range of motion, and functional disability. By offering a noninvasive and targeted intervention, this research seeks to improve movement quality and overall patient well-being.
Methodology:
A randomized clinical trial was conducted from May 2024 to December 2024 at Gulam Abbas orthopedic hospital, and DHQ hospital Kotli, Azad Kashmir. After approval of ethical committee of Riphah college of Rehabilitation and Allied Health Sciences, Riphah International University (REC/MS-PT/01879) and DHQ Kotli, Sample Size was calculated using G* power software with effect size 0.25, alpha error 0.05 and power 0.95 that was 36 which was randomly allocated in both groups, using Randomized control design technique.
Patients were included in the study from the Gulam Abbas Orthopedic Hospital and District head Hospital Kotli Azad Kashmir. Patients were randomly allocated in both groups, using randomized control design based on the inclusion criteria. Participants aged 30–50 years of either gender presenting with low back pain were included in the study. Eligible participants had pain and hypomobility due to lower-crossed syndrome, characterized by weak abdominal and gluteal muscles, tight hip flexors and erector spinae, a hyper lordotic lumbar curve, and anterior pelvic tilt greater than 7–10 degrees, while participants with musculoskeletal pathologies of the lower back, pelvis, hips, or lower limbs (such as herniated disc, lumbar radiculopathy, lumbar stenosis, or hip labral tear), patients unsuitable for spinal manipulation, pregnant individuals, and those with a history of spinal surgery, osteoporosis, or vertebral fractures were excluded from the study. Before beginning a treatment program, each patient received comprehensive information regarding the study and intervention, and they signed a written informed consent form in either English or Urdu, depending on their needs. A self-structured questionnaire was used to gather demographic data. Patients underwent assessments for pain at baseline and at the end of every week, and Range of motion of lumbar at baseline and at the end of 3rd week. Questionnaire comprised of demographics, Urdu and English consent forms, Numeric Pain Rating Scale (NPRS) with good reliability, strong construct validity (ICC: 0.86; 95 %CI, 0.33–0.96).8 And lumbar Range of Motion (Flexion, Extension, sidebend to right and left and rotation to right and left measured by goniometer having excellent reliability and validity ranging from 0.71 to 0.83.9 Intervention protocol given to Group A patients was Lumbar SNAGs, while they were sitting and standing, with six to eight repetitions per session, using anterocranial glide in the direction of the treatment plane across the spinous or transverse process, with 6 to 8 repetitions per sessions and moist hot pack along with stretching of tight erector spinae, hip flexors and strengthening of weak abdominals and gluteal muscles. Stretching exercises for tight erector spinae and hip flexors with 1 set of 5-7 reps with 5 second hold, 3 times a week, for total 3 weeks. For Strengthening of weak abdominals and gluteal muscles, 10 to 15 reps of 1 set, 3 times a week, for 3 weeks. Intervention protocol for Group B includes moist hot pack along with stretching of tight erector spinae, hip flexors and strengthening of weak abdominals and gluteal muscles. Stretching exercises for tight erector spinae, hip flexors with 5 second hold and 1 set of 5-7 reps 3 times a week, for 3 weeks. For Strengthening of weak abdominals and gluteal muscles, 10 to 15 reps of 1 set 3 times a week, for 3 weeks. Data was analyzed by using SPSS version 25. Shapiro-Wilk was used to verify the normality of data. Normality value of NPRS was <0.05 so Mixed way ANOVA was employed for between-group analysis of the NPRS. Normality value for Lumbar flexion extension, side bending and rotation was<0.05 soMann Whitney, U test was used to nalysed for between group analysis of lumbar ROMs, while within-group analysis was conducted using the Wilcoxen sign rank test for lumbar ROMs
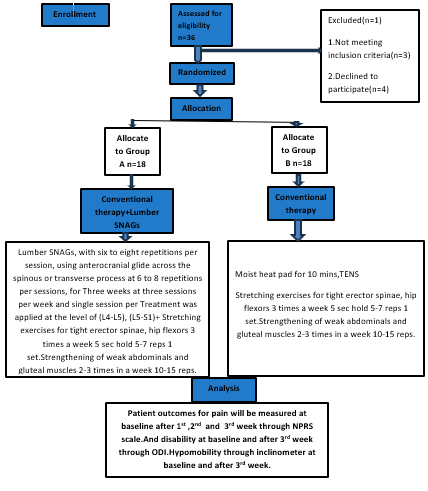
Figure 1: CONSORT Diagram
Results:
A total of 36 Participants were divided in to 2 groups with equal distribution of 18 participants in each group. Demographic profile of both groups is given in Table 1. Result of NPRS among groups, P values (0.01) of One-way ANOVA and P value (<0.001) of Post hoc test of NPRS shown in Table 2. Between groups analysis (Man Whitney U Test) p value (<0.001) of lumbar ROMS is given in Table 3. Within group analysis (WilcoxenTest) p value (<0.001) of lumbar ROMS is given in Table 4.
| Table 1: Demographic Profile | ||
| Demographic profile | Group A (n= 18) | Group B (n=18) |
| Male n (%) | 1 (5.56%) | 17(94.44%) |
| Female n (%) | 0 (0%) | 18(100%) |
| Age (Mean±SD) | 39.06±4.123 | 39.56±3.518 |
| BMI (Mean±SD) | 27.61±6.409 | 29.00±2.931 |
| Long sitting hours n (%) | Yes 14(77.8%) | Yes 9(50.0%) |
| No 4(22.2%) | No 9(50.0%) | |
| History of lumbar trauma n (%) | Yes 0(0%) | Yes 2(11.1%) |
| No 18(100%) | No 16(88.9%) | |
| Table 2: Mean± SD of NPRS among groups | ||||||
| Variable
|
Group A
Lumbar SNAGs +conventional therapy |
Group B
Conventional therapy |
P value
(Main Effect) One-way ANOVA |
P values
Group A Baseline-3rd week (Post Hoc Test–Repeated measure ANOVA) |
P values
Group B Baseline-3rd week (Post Hoc Test– Repeated measure ANOVA) |
|
|
NPRS |
Baseline | Mean ± SD | Mean ± SD | 0.18 | 0.01 | <0.001 |
| 1st week | 6.06 ± 1.05 | 6.44± 0.61 | 0.13 | <0.001 | <0.001 | |
| 2nd week | 5.17 ± 1.29 | 4.61 ± 0.85 | 0.06 | <0.001 | <0.001 | |
| 3rd week | 2.72 ± 1.07 | 3.50 ± 1.38 | 0.01 | <0.001 | <0.001 | |
| Table 3: Between group analysis (Man Whitney U test) on ROMS | |||||
| Variables | Assessments | Groups | Mean Rank
|
Median (IQR) | P-value |
| Lumbar Flexion ROM | Baseline | Group A | 20.39 | 37(10) | 0.27 |
| Group B | 16.61 | 35(10) | |||
| At 12th
session |
Group A | 25.92 | 60(0) | <0.001 | |
| Group B | 11.08 | 47(5) | |||
| Lumbar Extension ROM | Baseline | Group A | 18.11 | 30(2) | 0.79 |
| Group B | 18.89 | 30(02) | |||
| At 12th
session |
Group A | 22.42 | 35(0) | 0.01 | |
| Group B | 14.58 | 30(05) | |||
| Lumbar Rightside bending | Baseline | Group A | 19.19 | 15(7) | 0.67 |
| Group B | 17.81 | 15(10) | |||
| At 12th
session |
Group A | 25.00 | 25(0) | <0.001 | |
| Group B | 12.00 | 20(5) | |||
| Lumbar Leftside bending | Baseline | Group A | 20.64 | 20(7) | 0.18 |
| Group B | 16.36 | 15(10) | |||
| At 12th
session |
Group A | 25.44 | 25(0) | <0.001 | |
| Group B | 11.56 | 20(5) | |||
| Lumbar Rightside rotation | Baseline | Group A | 16.42 | 7(1) | 0.18 |
| Group B | 20.58 | 8(1) | |||
| At 12th
session |
Group A | 26.19 | 17(1) | <0.001 | |
| Group B | 10.81 | 14.5(1) | |||
| Lumbar Leftside rotation | Baseline | Group A | 17.56 | 8(1) | 0.54 |
| Group B | 19.44 | 8(1) | |||
| At 12th
session |
Group A | 26.28 | 17(2) | <0.001 | |
| Group B | 10.72 | 14(2) | |||
| Table 4: With in group analysis (Wilcoxen test) on ROMS | |||||||
| Variable
|
Group A
Mean Rank |
Group A
(Median (IQR) |
P value
(Wilcoxen test) |
Group B
Mean Rank |
Group B
Median (IQR) |
P value
(Wilcoxen test) |
|
| Lumbar Flexion ROM | Baseline-9th session | 9.0 | 37(10)
60(0) |
<0.001 | 8.0 | 35(10)
47(05) |
<0.001 |
| Lumbar Extension ROM | Baseline-9th
session |
8.0 | 30(02)
35(0) |
<0.001 | 3.50 | 30(02)
30(05) |
0.01 |
| Lumbar Right-side bending | Baseline-9th session | 8.50 | 15(07)
25(0) |
<0.001 | 4.00 | 15(10)
20(05) |
<0.001 |
| Lumbar Left side bending | Baseline-9th
session |
8.50 | 20(07)
25(0) |
<0.001 | 4.50 | 15(10)
20(05) |
<0.001 |
| Lumbar Right-side Rotation | Baseline-9th
session |
9.50 | 7(01)
17(01) |
<0.001 | 9.50 | 8(01)
14.5(01) |
<0.001 |
| Lumbar Leftside Rotation | Baseline-9th
session |
9.50 | 8(1)
17(02) |
<0.001 | 9.50 | 8(1)
14(02) |
<0.001 |
Discussion:
This study was conducted to see the effects of Lumbar sustained natural apophyseal glides on pain and hypomobility in patients with Lower cross syndrome. This study aimed to evaluate the effect of Lumbar SNAGS in decreasing pain and hypomobility in patients with Lower cross syndrome.
Between-group analysis of group A and B for variable NPRS showed that there was a significant difference between both groups, but lumbar Snags along with conventional therapy group showed more effective than conventional therapy alone When comparing the overall pain reduction from baseline to the 3rd week, both groups showed statistically significant and substantial improvements. Group A exhibited slightly greater pain relief This can be justified through the study conducted on effect of Mulligan concept lumbar SNAG on chronic nonspecific low back pain. Results shown significant improvement of Lumbar SNAG group as compared to therapeutic exercises group.10
Between-group analysis revealed a significant difference in lumbar flexion between Group A and Group B. Group A demonstrated significantly greater improvement in lumbar flexion ROM compared to Group B, indicating superior outcomes in the experimental group. Within-group analysis from baseline to the 3rd week further showed that lumbar SNAGs combined with conventional therapy were more effective in improving lumbar flexion ROM than conventional therapy alone. This can be justified through the study conducted on immediate effect of modified lumbar SNAGs in nonspecific chronic low back pain patients. Results shown significant improvement of Lumbar SNAG group as compare to therapeutic exercises group.10
Between-group analysis demonstrated a significant difference in lumbar extension between Group A and Group B, with Group A showing greater improvement in lumbar extension ROM. Within-group analysis from baseline to the 3rd week confirmed that lumbar SNAGs combined with conventional therapy were more effective in improving lumbar extension ROM than conventional therapy alone. This can be justified by a study immediate effect of two mulligan selected technique and results conclude a better improvement on lumbar extension ROM.7
Between-group analysis demonstrated a significant difference in lumbar right side and left bending between Group A and Group B, with Group A showing greater improvement in lumbar right and left side bending ROM. Within-group analysis from baseline to the 3rd week confirmed that lumbar SNAGs combined with conventional therapy were more effective in improving lumbar right and left side bending ROM than conventional therapy alone. This is supported by research SNAG’s with exercise and MFR with exercise offered short-term statistically significant improvements in pain, lumbar ROM.11
Between groups analysis of group, A and Group B for variable lumbar right and left side rotation shows that between group analysis of both groups had a significant effect. But. Group. A demonstrated significantly greater improvement in lumbar right and left side rotation ROM as compare to group B. This indicates that intervention applied to group A had better results as compare to group B. Within group analysis for variable lumbar right and left side rotation showed that Group A and B are effective in improving lumbar right and left side rotation. But group A showed a greater improvement. This is evident from study effect of lumbar sustained natural apophyseal glides with and without thoracic posture correction on mechanical low back pain, and study conclude that lumbar snags are effective in improving lumbar range of motions.12
Limitation: This study had a limited number of male participants due to ethical considerations. Additionally, treating Lumbar SNAGs were more difficult to apply consistently in obese patients due to challenges in palpating spinal landmarks and delivering precise mobilization forces, which may have reduced treatment accuracy and effectiveness. Future research should investigate the specific roles of pelvic tilt and lumbar lordosis in influencing treatment outcomes for Lower Cross Syndrome.
Conclusion:
The results of this research study indicate a significant difference between the effects of lumbar sustained natural apophyseal glides (SNAGs) combined with conventional therapy and conventional therapy alone. The study concludes that the integration of lumbar SNAGs with conventional therapy is more effective in reducing pain and improving lumbar range of motion compared to the use of conventional therapy alone. It is recommended that further researches should be done to explore how pelvic tilt and lumber lordosis influence outcomes. Future studies could include a post treatment three month follow up in order to check retention effects of the interventions.
References:
- Burile G, Phansopkar P, Deshmukh NS, Burile GC. Prevalence of Lower Cross Syndrome in Housemaids. Cureus. 2024;16(4).
- Sahu P, Phansopkar P. Screening for lower cross syndrome in asymptomatic individuals. J Med Pharm Allied Sci. 2021;10(6):3894-8.
- Kandil EA, Yamany AAER, Alsaka SSD, Abd El-Azeim AS. Effect of global postural reeducation on chronic low pain patients with lower cross syndrome. Bulletin of Faculty of Physical Therapy. 2024;29(1):8.
- Hartvigsen J, Hancock MJ, Kongsted A, Louw Q, Ferreira ML, Genevay S, et al. What low back pain is and why we need to pay attention. The Lancet. 2018;391(10137):2356-67.
- Ali I, Khan H, Rahman B, Nadir A, Khan HY, Ahmad M. Prevalence of lower cross syndrome and its association with bmi among nurses: a cross-sectional study. 2025.
- Edwards J, Hayden J, Asbridge M, Gregoire B, Magee K. Prevalence of low back pain in emergency settings: a systematic review and meta-analysis. BMC musculoskeletal disorders. 2017;18(1):143.
- Key J. The Pelvic Crossed Syndromes: A reflection of imbalanced function in the myofascial envelope; a further exploration of Janda’s work. Journal of bodywork and movement therapies. 2010;14(3):299-301.
- Young I, Dunning J, Escaloni J, Maselli F, Prall J, Mourad F, et al. Reliability, construct validity, responsiveness and minimum clinically important difference of the numeric pain rating scale and shoulder pain and disability index in patients with subacromial pain syndrome. Musculoskeletal Science and Practice. 2025:103372.
- Aburub AS, Alawna M, Mohamed AA, Nassif M. Using a smartphone goniometer to measure active thoracolumbar spine range of motion of lateral flexion and rotation among people with non-specific low back pain: a reliability and validity study. International Journal of Therapy And Rehabilitation. 2025;32(5):1-13.
- Hoy D, Bain C, Williams G, March L, Brooks P, Blyth F, et al. A systematic review of the global prevalence of low back pain. Arthritis & rheumatism. 2012;64(6):2028-37.
- Ishida H, Hirose R, Watanabe S. Comparison of changes in the contraction of the lateral abdominal muscles between the abdominal drawing-in maneuver and breathe held at the maximum expiratory level. Manual therapy. 2012;17(5):427-31.
- Clark RA, Mentiplay BF, Hough E, Pua YH. Three-dimensional cameras and skeleton pose tracking for physical function assessment: A review of uses, validity, current developments and Kinect alternatives. Gait & posture. 2019;68:193-200.
| Copyright Policy
All Articles are made available under a Creative Commons “Attribution-NonCommercial 4.0 International” license. (https://creativecommons.org/licenses/by-nc/4.0/). Copyrights on any open access article published by Journal Riphah college of Rehabilitation Science (JRCRS) are retained by the author(s). Authors retain the rights of free downloading/unlimited e-print of full text and sharing/disseminating the article without any restriction, by any means; provided the article is correctly cited. JRCRS does not allow commercial use of the articles published. All articles published represent the view of the authors and do not reflect the official policy of JRCRS. |